Amid the second wave of coronavirus in India, a rare fungal infection among COVID-19 patients has come to the fore now. The rare fungal infection is being referred to as Black Fungus or Mucormycosis. ICMR recently released an advisory stating that people on medication that reduces their ability to fight environmental pathogens will be mainly affected. It has been detected in COVID-19 patients with uncontrolled diabetes and prolonged Intensive Care Unit stay and this may turn fatal if uncared for.
Last year in New Delhi more than 20 cases of black fungus were reported from a single hospital in which half of the patients lost their eyesight and this year in May, the black fungus was found again among recovering or recovered Covid-19 patients in Maharashtra, Gujarat, and Delhi. The prevalence of the disease is estimated to be around 70 times elevated in India than in the rest of the world.
What is mucormycosis or black fungus?
The term mucormycosis comprises a distinctive group of infections caused by fungi, it was previously called zygomycosis. These fungi are common in nature, living on decaying vegetation and diverse organic substances. Although the fungi and spores of Mucorales show little inherent pathogenicity toward normal persons, they can initiate aggressive and ruminant infections under certain clinical conditions such as Ketoacidotic diabetes or patients with leukemia or lymphoma. These infections often result in dangerous long-term consequences for surviving patients as it poses difficult diagnostic and therapeutic challenges.
How black fungus enter the human body?
People might unknowingly inhale the fungal spores, normally human bodies know how to fight against them but it is difficult for people who are immunocompromised. Out of several ways the most common route is through inhalation where the spores enter the lungs via airways, any injury site is always an entry point or it could enter the system through food.
Types of mucormycosis
The fungal disease can be classified based on their site of infection, route of acquisition, and type of virulence exhibited by the fungus. Symptoms of rhinocerebral or sinus and brain mucormycosis include one-sided facial swelling, headache, nasal or sinus congestion, black lesions on the nasal bridge or upper inside of the mouth, sore jaw, and fever. In the case of pulmonary or lung mucormycosis, the patient suffers from fever, cough, severe chest pain, and shortness of breath as it affects the lungs.
Patients with cutaneous or skin mucormycosis get blisters or ulcers on the skin and the infected area may turn black including pain, excessive redness, and swelling around the patches. Gastrointestinal mucormycosis induces abdominal pain, nausea, vomiting, and gastrointestinal bleeding. Disseminated mucormycosis appears in people who are suffering from several diseases, medical conditions, or suffering from comorbidity such as diabetes.
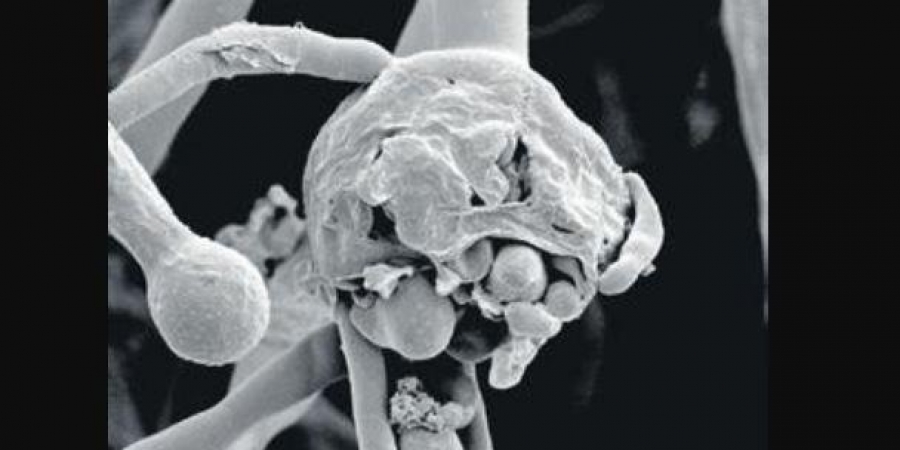
A magnified scan of Black fungus. (Representational Image)
Image Courtesy: www.newindianexpress.com
Why Mucormycosis is hitting COVID-19 patients
Black fungus is not harmful to people as human bodies have adapted themselves to handle the infection but individuals who are immunocompromised are more prevalent like patients who have undergone organ transplantation, stem cell transplantation, injury, or people who are using immunosuppressants like corticosteroid for a long time or people who are abusing drugs, consuming diabetic medications, undergoing chemotherapy. As this is a secondary infection, the chances of people with a good immune response are less and in case they catch the infection the suffering is almost negligible.
AIDS patients have a low count of T helper cells and patients suffering from coronavirus are more vulnerable as their immune systems are already into overdrive. Doctors have been prescribing steroids to cure the patients but at the same time, the steroids are reducing the immune response, weakening the body’s defense system, and increasing sugar levels, which becomes easier for the fungi to thrive off. It has also been reported in patients who were on ventilators in intensive care units, due to their airways being exposed to humidity and moisture.
How are black fungus cases treated?
The fungus doesn’t remain static after infecting a person, it spreads via the nose, attacks the eyes, and ultimately reaches the brain, at which point it becomes potentially deadly. Multi-discipline expertise is needed to treat it. In most cases, if the infection is undetected for long then different parts end up getting affected by mucormycosis. To save the patient’s life all infected tissues have to be surgically removed. In the process, some patients end up losing the eye/s and, in some cases, the upper jaw. After which patients are needed an intravenous antifungal procedure spanning four to six weeks.
Medicine for Black Fungus
Currently, India is treating patients infected with black fungus or mucormycosis with Amphotericin-B which is an antifungal drug. Due to shortage in drug five more pharma companies- Emcure Pharmaceuticals, Nacto Pharma, Gufic Bioscience Ltd., Alembic Pharmaceuticals, and Lyca Pharmaceuticals in India have got their drugs approved to increase the production in addition to the existing six pharma companies- Mylan, Bharat Serums, BDR Pharma, Sun Pharma, Cipla, and Life Care.
How to lower the risk of black fungus?
Mucormycosis is not contagious but one can lower the risk by avoiding construction or excavation sites and areas with dust, moisture, and fungi. If avoiding such places is not possible then one can reduce the chance of infection by wearing a mask and maintaining hygiene. Strengthening the immune system is also a way to fight back, eating a nutrition-rich diet is an efficient way to build a healthier immune system which will also help in clearing the fungal infection.
- COVID-19 Variant Omicron- A New Cause Of Concern
- Covid-19 Changing The Face Of Healthcare In India
- Impact Of COVID-19 On Early Childcare And Education
- Displaying Courage And Resilience: Women Combatting Covid-19
- Health And Hygiene- To Triumph Over Covid-19
- How Is The New Strain Of Covid-19 Impacting The World?




